It’s no secret that sadness is a natural part of human life. One may feel depressed or sad when going through a draining life experience or when a loved one passes away. These feelings tend to be temporary, so if they persist for long, it may indicate that one has a mental health condition such as major depressive disorder (MDD).
Also known as clinical depression, major depressive disorder can impact many aspects of one’s life. It affects behavior, mood, and physical functions like sleep and appetite.
With over
Symptoms of Major Depressive Disorder
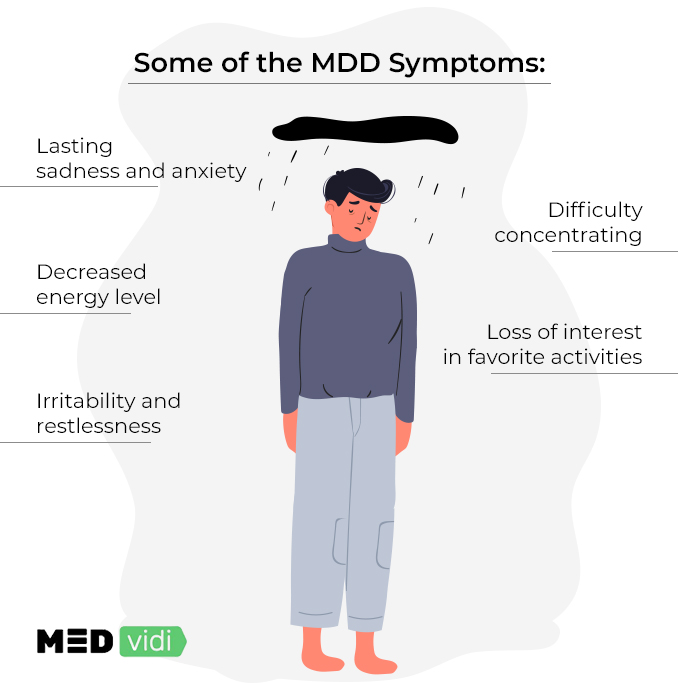
Depression is usually characterized by anhedonia and a feeling of sadness, stopping one from doing their everyday activities. As the disorder advances, the symptoms may be minor or severe. Though each person experiences major depressive disorder symptoms differently, here are the most common ones:
- Loss of interest in activities one enjoyed doing
- Lasting feelings of sadness or anxiety
- Weight and appetite changes
- Excessive sleeping or the inability to fall asleep
- Slowed speech, thinking, or physical activity
- Irritability and increased restlessness
- Decreased energy and tiredness
- Difficulty making decisions and concentrating
- Ongoing feelings of undue guilt or worthlessness
- Repeated thoughts of suicide and death
How MDD Is Treated
The right treatment may give someone with depression the tools and support they need to overcome sadness and hopelessness and feel motivated to be happy again. Major depressive disorder treatment can include one or a combination of these interventions:
Medicine
Since people with depression are believed to have low serotonin levels, SSRIs (selective serotonin reuptake inhibitors) are the common antidepressant type prescribed for MDD as they increase serotonin concentration in the brain. Serotonin is a neurotransmitter (brain chemical) that helps induce healthy sleeping patterns and improve mood. Examples of well-known SSRIs include citalopram (Celexa) and fluoxetine (Prozac).
Besides SSRIs, SNRIs (serotonin and norepinephrine reuptake inhibitors) such as venlafaxine (Effexor XR) and duloxetine (Cymbalta) can be prescribed for MDD. They prevent the reabsorption of norepinephrine and serotonin, which are needed to improve mood.
Other FDA-approved drugs to treat MDD include bupropion (Wellbutrin), mirtazapine (Remeron), trazodone (Desyrel), and Nefazodone (Serzone). The choice of medication will ultimately be at the peril of the doctor depending on one’s medical history, the severity of the condition, and suitability to a particular drug. Doctors also weigh the benefits and side effects of the drug before giving them to patients.
One should never assume they can stop taking depression medicine when they start feeling better. It’s always important to talk to a doctor before coming off the medication since quitting suddenly can increase the risk for withdrawal symptoms, relapse, or dysthymia.
Psychotherapy
Psychotherapy focuses on changing the negative or distorted views one may have on themselves or a situation. It also helps identify and manage the main stressors in one’s life and strengthen relationships.
Regularly talking to a therapist can help one learn skills for coping with negative emotions and thinking patterns. The psychotherapy sessions allow one to open up about issues in their life that are making them feel hopeless.
Psychotherapists have formal training and experience in several techniques that can help people resolve deeply-rooted personal issues, recover from mental disorders, and make positive changes in their lives. They employ different psychological and verbal techniques based on the client’s individual needs for quick recovery.
The most common psychotherapy method used to treat MDD is cognitive-behavioral therapy (CBT). It is carried out on the idea that people’s thoughts may impact their emotions. Though it is short-term and goal-oriented, it comes with long-lasting results. CBT helps patients to learn to identify patterns of cognitive distortions (negative thinking) and to turn these distortions into more positive ones to improve mood. Having a behavioral element, CBT also aids one in working on an emotional response to different situations and helps them to engage in productive activities again to enhance their overall well-being.
Self-Care Practices to Manage MDD Symptoms
MDD can make one feel hopeless, helpless, worthless, and exhausted. This can be dangerous in many ways, including the inability or lack of motivation to seek help. However, certain self-care practices and lifestyle changes can help one eliminate the symptoms of MDD to get ready to ask a doctor for professional help. These practices include the following:
- Socializing and confiding in someone
- Setting priorities and breaking large tasks into small ones
- Doing things that bring joy, such as gardening, watching a movie, or taking part in a charitable cause
- Exercising regularly
- Eating healthy, well-balanced meals
- Staying away from drugs and alcohol
However, the above tips can only serve as extra support. It is recommended to see a healthcare provider as soon as the MDD symptoms present, not trying to treat such a serious condition by yourself. A mental health professional will make a proper diagnosis, help you set realistic goals about the treatment outcomes, and will provide you with an effective treatment plan.
Summing Up
While one may feel hopeless at times as they struggle with MDD, it’s important to note that there are treatment interventions for the disorder. One should stick to the prescribed treatment plan for the best outcomes. And on days one feels depressed despite getting treated, they should speak to a mental health professional or local crisis service for help.